- Periodontal Health Guide
Bleeding gums aren’t normal — they’re a warning sign. Learn how gum disease develops, what modern treatment looks like, and how to stop it before it becomes serious.
Fighting Back: Modern Treatments for Gum Disease in Williamsburg
If your gums bleed when you brush, you’ve probably told yourself it’s nothing — maybe you were brushing too hard, or it “just happens.” But persistent bleeding is one of the clearest early signs of gum inflammation, and ignoring it tends to make the problem worse over time. The good news: treatment for gum disease has come a long way, and catching it early usually means simpler care than waiting until it progresses.
Gum disease — ranging from mild gingivitis to advanced periodontitis — is more common than many people realise. It often develops quietly without significant pain, which is part of why it can reach a more serious stage before people seek care. What starts as plaque buildup irritating the gums can, if left unaddressed, eventually affect the bone that supports the teeth.
The Rise of NY Cosmetic Dentistry: Your Options
Most gum problems begin with gingivitis — a mild early-stage inflammation largely caused by plaque accumulation along and just below the gumline. Plaque is a soft, sticky film of bacteria that forms on teeth throughout the day. When it isn’t removed consistently, it hardens into tartar (calculus) — a rough mineralised deposit that can’t be removed at home and provides a surface for more bacteria to collect.
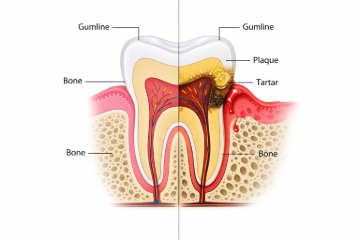
Bacteria in plaque and tartar irritate gum tissue and trigger inflammation. Gums become red, swollen, and more likely to bleed during brushing or flossing. The critical point: at the gingivitis stage, damage is limited to soft tissue — bone and ligaments are not yet affected. That’s why gingivitis is often reversible with professional cleaning and improved home care.
Gingivitis vs. Periodontitis: What's the Difference?
Gingivitis and periodontitis aren’t the same condition. They represent different stages of gum disease with very different implications for treatment and reversibility.
- GINGIVITIS
- Inflammation limited to gum tissue only
- No bone loss at this stage
- Often fully reversible with treatment and consistent home care
- Typically responds well to a professional cleaning plus improved daily habits
- PERIODONTITIS
- Infection spreads below the gumline into supporting structures
- Periodontal ligament and jawbone become involved
- Bone loss, once it occurs, cannot be reversed with standard treatment
- Can progress without obvious pain — often discovered at exam
IMPORTANT
The transition from gingivitis to periodontitis doesn’t happen overnight, but it can happen without obvious pain. Many people are surprised to learn they have early or moderate periodontitis because they haven’t felt significant discomfort.
Gum Disease Stages at a Glance
| Stage | Key Signs | Typical Treatment | Reversible? |
|---|---|---|---|
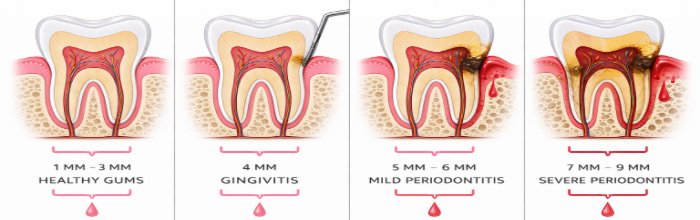
| Healthy Gums | Pink, firm, no bleeding. Pocket depth ~1–3 mm | Routine cleanings + strong home care | N/A (maintenance) |
| Gingivitis | Red/puffy gums, bleeding when brushing or flossing, no bone loss yet | Professional cleaning + improved home care | Often reversible |
| Mild Periodontitis | Pocket depths ~4–5 mm, early bone loss on X-ray, persistent bleeding | Scaling & root planing, sometimes localized antibiotics | Bone loss not reversible; progression can be controlled |
| Moderate Periodontitis | Pockets ~5–7 mm, visible gum recession, sensitivity, bad breath | Scaling & root planing, closer maintenance, possible specialist referral | Manageable and stabilisable |
| Severe Periodontitis | Pockets 7 mm+, significant bone loss, loose teeth, tooth loss risk | Advanced periodontal therapy, possible surgery, specialist co-management | Requires ongoing management |
Pocket depths and staging are confirmed during a clinical exam and may vary by individual case.
Symptoms You Shouldn't Dismiss
BLEEDING GUMS ARE NOT NORMAL
Persistent gum bleeding is a sign of active inflammation — not just “brushing too hard.” None of the symptoms below should be dismissed as “just how my mouth is.”
- Gums that bleed during brushing or flossing, especially for more than a week or two
- Persistent bad breath (halitosis) that doesn't improve with regular brushing and rinsing
- Gums that look redder, puffier, or more tender than usual
- Gum recession — teeth appearing longer than they used to
- Pus or discharge near the gumline
- Teeth that feel loose or have shifted position
- A persistent bad taste in the mouth that doesn't go away
- Sensitivity at the gumline, especially to cold or when eating
Advanced Treatment: Scaling & Root Planing (Deep Cleaning)
Once gum disease progresses beyond gingivitis — meaning gum pockets deepen and infection spreads below the gumline — a standard cleaning isn’t enough. The most common non-surgical treatment is scaling and root planing, often called a deep cleaning.
Despite the clinical name, scaling and root planing is a well-established procedure that typically does not involve cutting or suturing. It’s a more thorough cleaning of the root surfaces and pocket areas below the gumline that routine cleanings can’t reach.
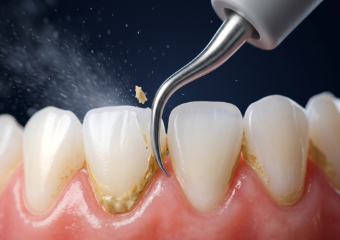
Scaling
Removing plaque, tartar, and bacterial deposits from tooth surfaces — including below the gumline and inside gum pockets. Both hand instruments and ultrasonic scalers may be used.
Root Planing
Smoothing root surfaces after scaling. Rough root surfaces trap bacteria, so smoothing helps reduce re-accumulation and supports healthier tissue reattachment over the following weeks.
When Localized Antibiotics or Medicated Rinses May Be Used
In some cases, deep cleaning alone isn’t enough to fully control bacterial activity in deeper pockets. A dentist or periodontist may recommend adjunctive therapy — such as localized antibiotics placed directly in a pocket, or a prescription antimicrobial rinse for short-term use. Whether this is needed depends on pocket depth, severity, health history, and how tissues respond after deep cleaning.
What to Expect After Deep Cleaning
Day 1-3
Immediate Post-Treatment
Some sensitivity and mild soreness is normal, especially to cold temperatures. Gums may look slightly more receded as swelling reduces — this is expected, not worsening recession.
Week 1-2
Inflammation Begins Resolving
Bleeding during brushing typically starts decreasing. This is the window where consistent home care has the most impact — brushing at the gumline and flossing daily accelerates tissue recovery.
Week 2-4
Noticeable Improvement
Many patients notice significantly less bleeding and inflammation within 2–4 weeks. Bad breath often decreases substantially once bacterial deposits are removed and infection is controlled.
Week 4-8
Follow-Up Re-Evaluation
Pocket depths are re-measured. In many cases, inflammation reduces and tissues firm up, which can decrease pocket measurements. Ongoing maintenance (every 3–4 months) is typically recommended.
Why Gum Health Is the Foundation of Your Smile
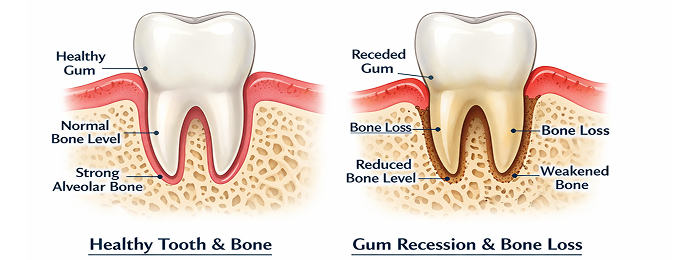
Gums and supporting bone are the foundation of oral health. You can have cavity-free teeth — but if the tissue and bone holding them in place are compromised, the teeth themselves are at risk. Gum disease is a major reason adults lose teeth, and much of that tooth loss is preventable when disease is identified and managed early.
There is also ongoing research into links between periodontal health and systemic conditions like cardiovascular disease, diabetes management, and pregnancy outcomes. The evidence supports an association — though it would be overstating it to describe gum disease as a direct cause of these conditions.
- Progressive bone loss compromising tooth stability
- Gum recession increasing sensitivity and root-surface decay risk
- Tooth mobility and tooth loss in advanced cases
- Persistent infection and inflammation over time
- More difficult home care as pockets deepen further
- Reduced longevity of cosmetic and restorative work if gums are unstable
Preventing Periodontitis with Simple Daily Habits
The best way to treat gum disease is to prevent it from progressing. Most of what protects your gums happens at home, not in the dental chair.
Brush Correctly, Twice Daily
2 minutes with a soft-bristled brush. Angle the brush 45° toward the gumline — that’s where plaque collects. Electric brushes can help.
Floss or Use Interdental Brushes Daily
Especially important before bed. Floss or interdental brushes reach areas where plaque builds between teeth and below the gumline.
Keep Maintenance Appointments
Routine cleanings every 6 months — or every 3–4 months if you have a history of periodontitis. Professional removal of tartar cannot be replicated at home.
Avoid Smoking & Tobacco
Tobacco use significantly increases gum disease risk and slows healing after treatment. It can also mask bleeding, making disease harder to detect early.
Use an Antimicrobial Rinse If Recommended
Not everyone needs one — but if your dentist recommends an antimicrobial or fluoride rinse as part of your home routine, use it consistently as directed.
Replace Your Toothbrush Regularly
Every 3 months, or sooner if bristles are worn. A worn brush doesn’t clean effectively along the gumline — the most critical area to reach.
What to Expect After Deep Cleaning
Materials
High blood sugar makes infections harder to control. Gum health and diabetes management influence each other bidirectionally.
Medications
Some cause dry mouth or gum overgrowth, both of which raise gum disease risk. Always share your medication list with your dentist.
Stress
Genetic
Specialised Periodontal Care in Williamsburg, Brooklyn
A routine cleaning is not the same as a periodontal exam. If you’ve been experiencing bleeding, recession, persistent bad breath, or gum tenderness, you deserve a thorough evaluation — not just a polish.
At Toothology in Williamsburg, a periodontal exam typically includes pocket depth measurements around each tooth, assessment of gum colour and recession, and dental X-rays when clinically indicated to evaluate bone levels.
Who Should Book a Periodontal Exam
- Your gums bleed for more than a week or two during brushing or flossing
- Bad breath persists despite regular brushing and rinsing
- You notice recession or your teeth looking longer than before
- Teeth feel loose or have shifted position
- You have higher-risk history — diabetes, smoking, immunosuppression, or certain medications
- It has been more than a year since your last cleaning or dental exam
- A prior dentist noted gum concerns and you haven't followed up since
PERSONALISED TREATMENT PLANNING
A 28-year-old with localised gingivitis needs a different plan than a 52-year-old with generalised moderate periodontitis. After your exam, your plan should clearly explain your stage, recommended treatment, timeline, maintenance schedule, and what to watch for at home.
Frequently Asked Questions
How to get rid of gingivitis?
Gingivitis is often reversible. The first step is a professional cleaning to remove tartar you can’t remove at home. Consistent brushing at the gumline, daily flossing/interdental cleaning, and any recommended rinse help the tissue heal.
How to treat gum disease?
Treatment depends on the stage. Gingivitis is usually treated with a professional cleaning and better daily habits. Periodontitis typically requires scaling and root planing (deep cleaning) to remove deposits below the gumline, followed by ongoing maintenance.
What causes gum disease?
Plaque is the primary cause. When plaque isn’t removed, it hardens into tartar and triggers inflammation. Risk factors include tobacco use, diabetes, certain medications, genetics, dry mouth, and immune-related conditions.
Is gum disease curable?
It depends. Gingivitis is often reversible. Periodontitis isn’t “curable” in the sense that bone loss cannot be restored through standard care, but it can often be managed and stabilized with proper treatment and maintenance.
How do you shrink gum pockets?
Deep cleaning removes deposits inside pockets; as inflammation resolves, tissue can firm and pocket measurements often decrease. Deeper pockets may require advanced periodontal care. Follow-up measurements determine the next steps.
What happens if periodontal disease goes untreated?
A periodontist is a specialist trained in diagnosing and treating gum disease and placing implants. They may manage advanced cases and procedures such as gum grafts, bone regeneration, and periodontal surgery.
What does a periodontist do?
Periodontitis progresses – pockets deepen, bone loss increases, teeth loosen, and tooth loss becomes more likely. Early treatment is far easier than managing late-stage disease.
CONCERNED ABOUT YOUR GUMS?
Book a periodontal exam at Toothology in Williamsburg. We’ll measure pocket depths, assess recession, and give you a clear, honest picture of what’s happening.
CALL US DIRECTLY
IN THIS GUIDE
TOOTHOLOGY DENTAL
Williamsburg, Brooklyn, NY
Serving Greenpoint, Bushwick, Bed-Stuy & Downtown Brooklyn
718-678-3800
Emergency line available
Open Hours
Mon – Thu: 10:00 AM – 6:00 PM Friday: 10:00 AM – 2:00 PM Sunday: 10:00 AM – 2:00 PM Saturday: Closed
OUR COMMITMENT
- Board-Certified Pediatric Dentists
- Child-Friendly, Anxiety-Reducing Care
- Same-Day Emergency Slots
- Low-Radiation Digital X-Rays
- Most Major Insurance Accepted
