- Restorative Dentistry Guide
Root Canal vs. Extraction
Save it or remove it? Both can be the right call — but the decision depends on more than just pain. Here’s how to think it through.
When a tooth is causing serious pain, almost every patient asks the same question: Should I save it, or just have it pulled? The debate over root canal vs. extraction is one of the most common decisions in dentistry — and it rarely has a simple answer.
What’s true is that both options can be the right choice in the right circumstances. Root canals aren’t always the heroic tooth-saving solution, and extractions aren’t always the “quick shortcut.” The best decision depends on the condition of the tooth, the surrounding bone, your overall oral health, your budget, and your long-term goals for your smile.
Saving Your Natural Tooth: The Benefits of a Root Canal
Dentists generally prefer saving a tooth when it’s realistically possible — and for good reason. Natural teeth aren’t just tools for chewing; they’re part of a system that includes your jawbone, bite alignment, and the stability of nearby teeth. Losing a tooth can trigger changes that become inconvenient and costly later
A root canal removes infected or damaged tissue from inside the tooth (the pulp chamber and root canals) while keeping the outside structure intact. After the infected tissue is removed, the tooth is cleaned, shaped, sealed, and typically restored with a crown.
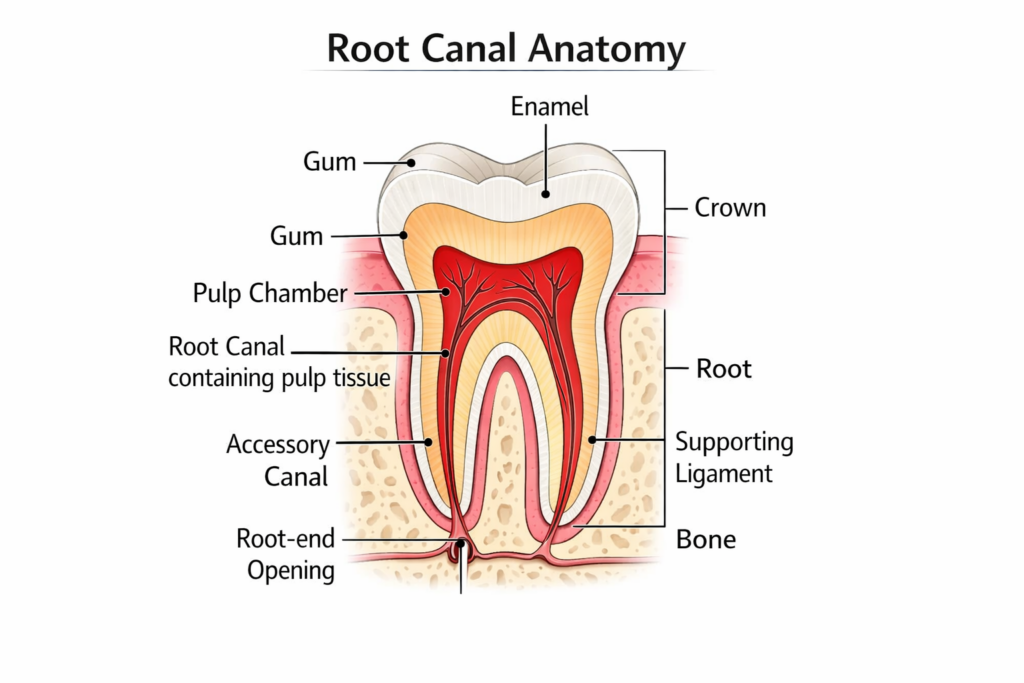
When Is a Root Canal Typically Recommended?
Root canal treatment is generally recommended when the pulp — the soft tissue inside the tooth containing nerves and blood vessels — has become infected or irreversibly inflamed, but the tooth is still structurally restorable. Common causes include:
- Deep cavities that reach the pulp
- A cracked tooth that exposes the pulp
- Trauma that damages the nerve
- Multiple procedures on the same tooth over time
Key Qualifier — Restorability
If a tooth is fractured below the gumline or too compromised to support a crown, a root canal is usually not the best path regardless of the infection status.
- PROS OF A ROOT CANAL
- Preserves your natural tooth, supporting jawbone health and bite balance
- Eliminates infection and relieves pain while keeping the tooth in place
- Avoids the immediate gap that comes with extraction
- Often a faster return to normal chewing than extraction + replacement
- Natural teeth typically feel more stable than removable options
- CONS & LIMITATIONS
- A crown is usually needed afterward — added cost and another step
- Eliminates infection and Root-canal-treated teeth can become more brittle over time pain while keeping the tooth in place
- May require retreatment in some cases
- Not suitable for severely fractured or non-restorable teeth
- Complex cases may require an endodontist (specialist)
When Is a Tooth Extraction the Better Option?
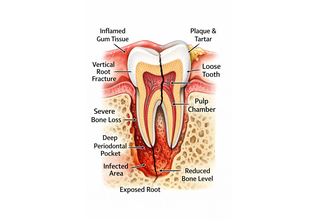
Saving a tooth is often the goal, but not every tooth can or should be saved. Choosing extraction when it’s clearly indicated isn’t “settling” — in many situations, it’s the safest and most predictable decision.
Extraction decisions should be based on a thorough exam with X-rays and, when helpful, vitality testing — not assumptions or symptoms alone.
When Extraction Is Generally the Better Choice
Vertical root fracture
A crack running along the root is not repairable; extraction is usually recommended.
Severe decay below the gumline
Too little tooth remains to hold a crown predictably.
Advanced bone loss from periodontal disease:
A tooth may be too mobile or compromised to remain functional.
Non-restorable anatomy/structure:
Some teeth are too compromised for predictable root canal success.
Failed root canal + weak structure:
If retreatment isn't feasible due to structural compromise, extraction may be the better option.
- PROS OF EXTRACTION
- Removes the source of infection or pain quickly
- Often simpler and less time-intensive than complex root canal therapy
- May be the most practical option for heavily compromised teeth
- Can be less expensive upfront (especially if replacement is delayed)
- LONGER-TERM CONSEQUENCES
- Leaves a gap; nearby teeth can shift over time
- Jawbone can resorb (shrink) without a root or implant stimulation
- Chewing efficiency and bite balance may change
- Replacement (implant, bridge, partial) adds cost and additional visits
- Total cost of extraction + replacement can exceed root canal + crown
Comparing the Long-Term Costs
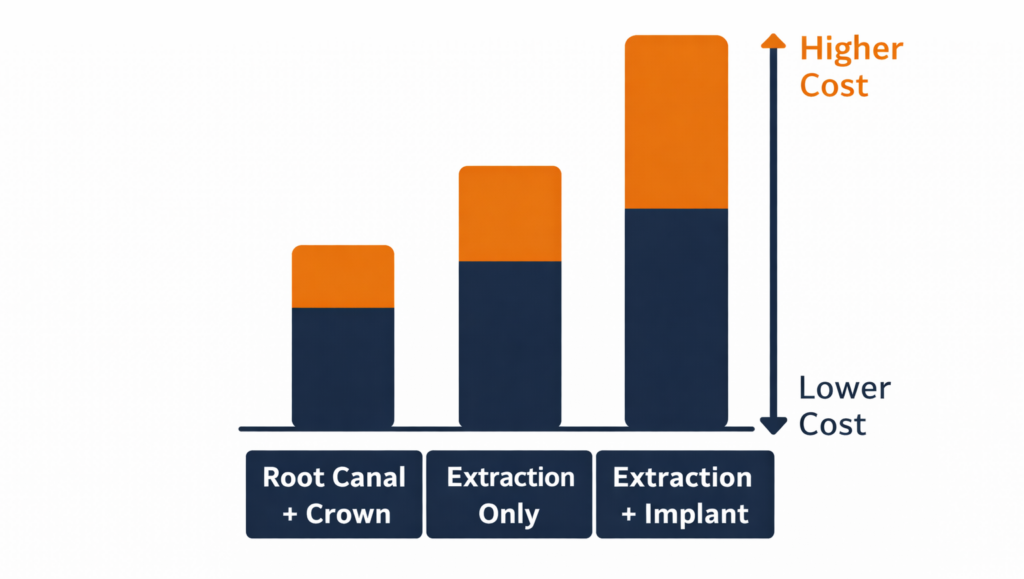
Cost is a common reason people lean toward extraction. A root canal typically includes the procedure plus a crown afterward — the crown is often essential, as without it the tooth is more vulnerable to fracture.
Extraction often looks cheaper upfront, but if you plan to replace the tooth, the total treatment can include an implant or bridge and sometimes bone grafting. When replacement is factored in, extraction may cost more long-term.
Root Canal vs. Extraction at a Glance
| Factor | Root Canal | Extraction |
|---|---|---|
| Goal | Save the natural tooth | Remove the tooth entirely |
| Pain Relief | Often improves within days | Often immediate once tooth is removed |
| Tooth Preserved? | Yes — crown placed afterward | No — gap remains unless replaced |
| Number of Visits | Often 1–2 visits + crown | 1 visit for extraction; more if replacing |
| Bone Loss Risk | Low — natural root helps maintain bone | Higher — bone resorbs without replacement |
| Shifting Teeth | Unlikely — tooth remains in place | Possible without replacement |
| Long-Term Durability | Can last many years with crown + care | Depends on replacement chosen |
| Replacement Needed? | No | Often yes — implant, bridge, or partial |
| Cost Drivers | Root canal + crown; possible specialist | Extraction + replacement; possible grafting |
| Best For | Restorable infected or decayed tooth | Non-restorable tooth, severe fracture, advanced bone loss |
Restoring Your Smile with Implants After an Extraction
If a tooth is extracted, the story shouldn’t end there. The gap isn’t only cosmetic. Over time, the jawbone in that area can lose density without stimulation — a process called resorption.
Bone Grafting at the Time of Extraction
Socket preservation (bone grafting immediately after extraction) may help maintain ridge shape and volume. It’s not always necessary, but if an implant is part of the long-term plan, preserving bone can make future implant placement easier and more predictable.
Choosing the Right Replacement: Implant, Bridge, or Partial
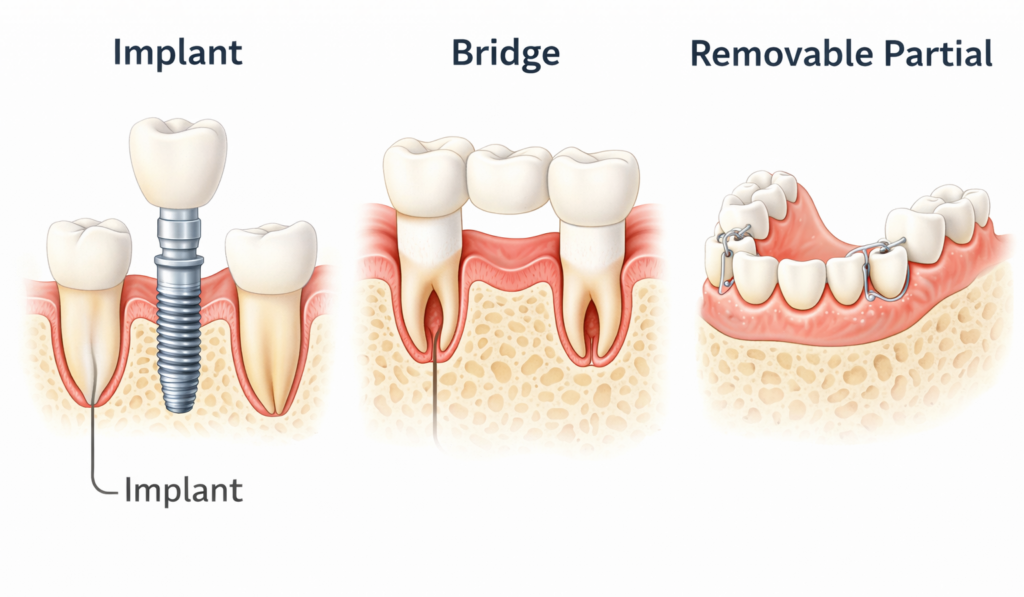
| Option | Best For | Pros | Cons | Timeline |
|---|---|---|---|---|
| Dental Implant | Single missing tooth with adequate bone | Feels natural, preserves bone, very durable | Higher upfront cost; surgical healing time required | Several months total |
| Dental Bridge | 1–2 missing teeth; adjacent teeth already need crowns | Non-surgical, faster than implant | Requires prepping adjacent teeth; doesn't prevent bone loss under the gap | 2–3 visits over weeks |
| Removable Partial | Multiple missing teeth; budget-conscious patients | Lower upfront cost; no surgery needed | Less stable; may feel less natural; periodic adjustments needed | A few weeks |
Why a Diagnostic Exam Matters

The decision between root canal and extraction shouldn’t be made based on an internet search alone. The right choice depends on information only a clinical exam can provide: X-rays, structural assessment, bone evaluation, and sometimes pulp vitality testing.
For patients in Williamsburg, Greenpoint, Bushwick, and surrounding North Brooklyn neighborhoods, consulting a dentist — and, when needed, an endodontic specialist — helps you make a safe decision based on prognosis, not guesswork.
What a Diagnostic Exam Actually Involves
Clinical Examination
Evaluating the tooth and surrounding tissue for infection, swelling, and structural compromise.
Diagnostic X-Rays
Assessing roots, infection extent, bone level, and existing root canal work.
Vitality Testing
When indicated, confirming if the nerve is alive, dying, or non-vital.
Prognosis Conversation
Realistic expectations, risks, and long-term implications of each option discussed openly.
WHAT TO BRING TO YOUR APPOINTMENT
- Insurance card and any coverage details you have
- Symptom timeline — when pain started, triggers, prior treatment
- Current medications and known allergies
- Any recent X-rays if you were seen elsewhere first
Frequently Asked Questions
Is it better to get a root canal or tooth extraction?
It depends on the condition of the tooth. If the tooth is structurally restorable and the issue is primarily within the pulp, a root canal is often preferred because it preserves the natural tooth and avoids replacement. If the tooth is non-restorable due to fracture, severe decay, or major bone loss, extraction is usually the safer option. An exam with X-rays is the best way to decide.
What is cheaper, a root canal or extraction?
Extraction is usually cheaper upfront, but the full cost depends on whether you replace the tooth. If you plan an implant or bridge, extraction plus replacement often costs more than a root canal and crown.
Does a root canal hurt more than an extraction?
Neither procedure should be painful during treatment—both are performed with local anesthesia.
When should you pull a tooth instead of doing a root canal?
Extraction is often recommended for vertical root fractures, non-restorable decay below the gumline, severe periodontal bone loss, or when a previously treated tooth has a poor structural prognosis for retreatment.
Are root canals worth it?
For the right tooth, yes. Root canals can eliminate infection and preserve a tooth for many years when properly restored and maintained.
How long can a dead tooth stay in your mouth?
A non-vital (dead) tooth may remain without obvious symptoms for a time, but that doesn’t mean it’s safe to leave untreated. It can become infected, weaken structurally, or develop an abscess that affects surrounding bone.
Can a tooth that needs a root canal heal itself?
No. Once the pulp is irreversibly inflamed or infected, it cannot heal on its own.
What happens if you do not get a root canal?
If a tooth that needs root canal treatment is left untreated, the infection often progresses. This can lead to an abscess, spreading infection, damage to surrounding bone, and eventual loss of the tooth.
NOT SURE WHICH WAY TO GO?
Book a diagnostic exam and let our team review your X-rays and walk you through your options — no pressure.
CALL US DIRECTLY
IN THIS GUIDE
TOOTHOLOGY DENTAL
Williamsburg, Brooklyn, NY
Serving Greenpoint, Bushwick, Bed-Stuy & Downtown Brooklyn
718-678-3800
Emergency line available
Open Hours
Mon – Thu: 10:00 AM – 6:00 PM Friday: 10:00 AM – 2:00 PM Sunday: 10:00 AM – 2:00 PM Saturday: Closed
OUR COMMITMENT
- Board-Certified Pediatric Dentists
- Child-Friendly, Anxiety-Reducing Care
- Same-Day Emergency Slots
- Low-Radiation Digital X-Rays
- Most Major Insurance Accepted
