- Gingivitis & Gum Health Guide · Brooklyn
A tinge of pink in the sink. Tender gums you’ve been brushing off for months. Here’s why bleeding gums matter — and what early action actually looks like.
Are Your Gums Bleeding? Why You Shouldn't Ignore Early Gingivitis
You rinse after brushing and notice a tinge of pink in the sink. You floss carefully and your gums bleed again. The tenderness along the gumline has been there for a while, but you’ve been telling yourself it’s probably nothing serious. It’s worth paying attention to.
Bleeding gums are one of the most common early signs of gum disease. The reassuring part is that, when caught early, gingivitis is usually reversible with professional care and improved home hygiene. The problem is that many people wait until symptoms have clearly worsened before seeing a dentist — and by then, treatment is often more involved.
Why Do Gums Bleed? Common Triggers and Risks
Bleeding gums are not something you should normalise. Healthy gums do not usually bleed during normal brushing or flossing. When they do, the gum tissue is often inflamed or irritated.
The most common reason is plaque buildup. Plaque is a sticky film of bacteria that forms on teeth every day. If it isn’t removed consistently, it can irritate the gums and trigger inflammation — making the tissue redder, puffier, more tender,
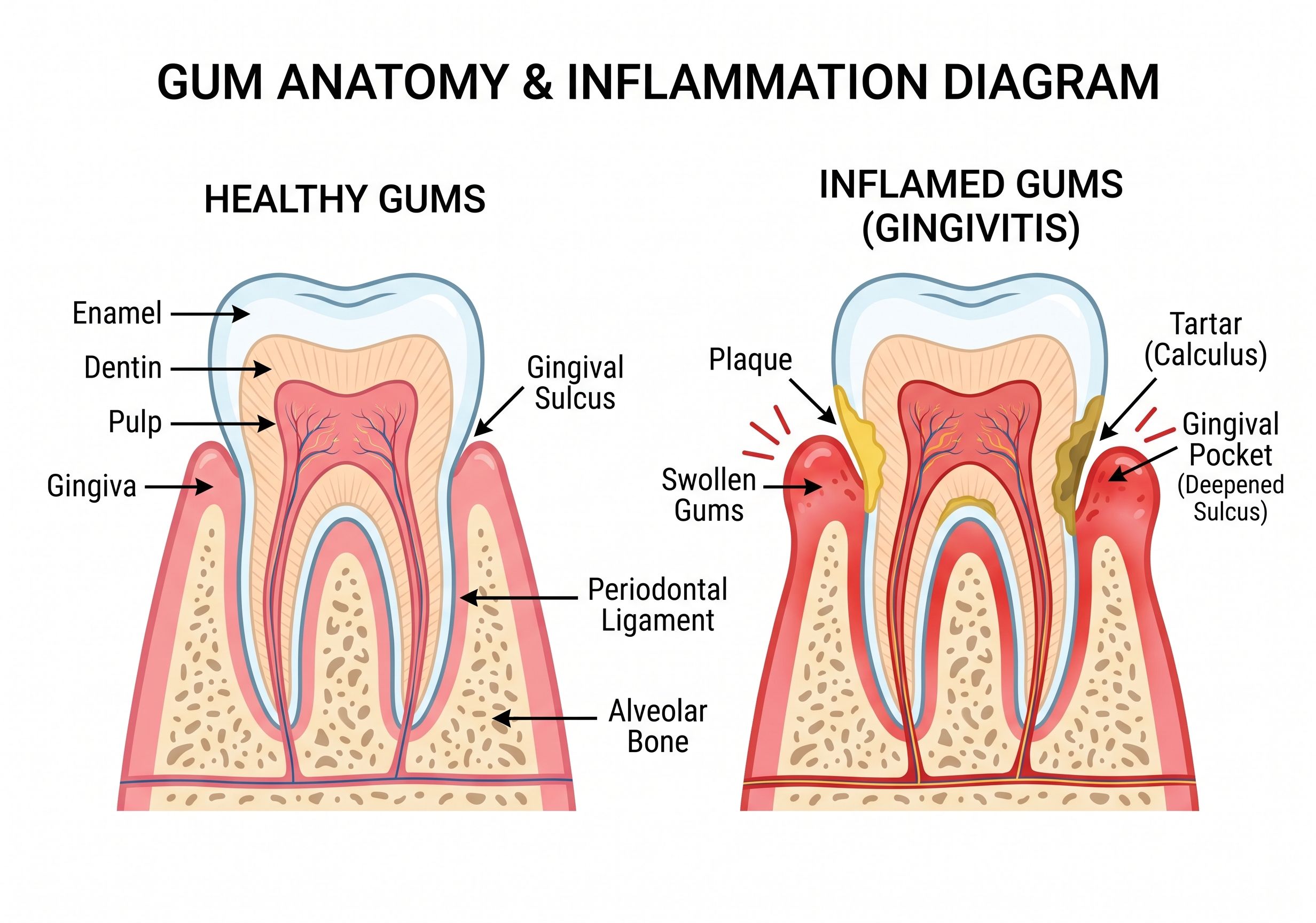
and more likely to bleed. Over time, plaque can harden into tartar, which can’t be removed by brushing alone.
Other Contributing Factors
Brushing too hard or with a worn, stiff-bristled toothbrush
Not flossing consistently — especially if restarting after a gap
Hormonal changes — pregnancy, menopause, or hormonal shifts
Certain medications that cause gum overgrowth or dry mouth
Smoking or tobacco use — which can mask bleeding and worsen inflammation
Dry mouth — reduces saliva that helps protect gum tissue
Systemic conditions such as diabetes — linked to higher gum disease risk
Genetics — some people are more susceptible regardless of hygiene habits
THE SIMPLE RULE
If your gums bleed repeatedly during ordinary home care, it’s worth getting checked. A single bleeding episode after aggressive flossing is different from a consistent pattern over weeks.
Early Signs of Gingivitis You Shouldn't Ignore
One of the frustrating things about gingivitis is that it’s often painless at first. Many people assume that if they’re not in obvious pain, nothing serious is happening. That’s not always true — and it’s exactly why so many cases of gingivitis progress further than they need to.
Gums that bleed when brushing or flossing — especially if this happens consistently
Red, swollen, or tender gums — particularly along the gumline
Persistent bad breath or a bad taste that doesn't improve with brushing
Puffiness or changes in the gum texture along the gumline
Gums that seem to be pulling back or receding — teeth looking longer than before
Gum sensitivity that makes brushing or eating uncomfortable
A REPEATED PATTERN MATTERS MORE THAN ONE SYMPTOM
A single symptom doesn’t confirm a diagnosis, but a repeated pattern — especially bleeding that keeps coming back — should not be dismissed. Early gingivitis that gets addressed promptly is much simpler to treat than disease that has had time to progress.
Gum disease usually begins with plaque. If plaque isn’t removed, it can harden into tartar — which brushing alone cannot remove. As bacteria and tartar collect along and below the gumline, inflammation continues and can deepen over time.
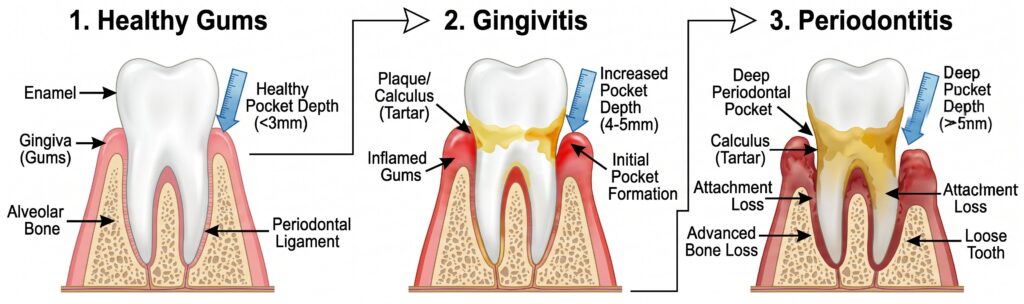
HEALTHY GUMS
Pink, firm, not tender. No bleeding during normal brushing or flossing. Pocket depths within normal range (~1–3mm). Maintained with consistent home care and regular professional cleanings.
VITIS
GINGIVITIS
Inflammation limited to the gum tissue. Red, puffy, tender gums that bleed easily. No bone loss at this stage. Usually reversible with professional cleaning and improved daily home care. The right time to act.
DONTITIS
PERIODONTITIS
Infection spreads deeper, affecting the structures supporting the teeth. Gum pockets deepen, bone loss begins. More involved treatment is needed — scaling and root planing, and ongoing periodontal maintenance. Bone loss is not reversible with standard treatment.
WHY EARLY ACTION MATTERS
Treating gingivitis is usually simpler than managing established periodontitis. The window for reversibility is real — but it closes as disease progresses. Getting checked early keeps the most manageable options on the table.
What Gum Disease Treatment in Brooklyn May Look Like
If you come to Toothology with bleeding gums, tenderness, or concern about recession, the first step is evaluation — not assumptions. The level of care recommended depends on what the exam shows.
What a Typical Evaluation Includes
CLINICAL GUM EXAMINATION
Visual assessment of gum tissue colour, texture, recession, and swelling around all teeth.
PERIODONTAL MEASUREMENTS
Pocket depth measurements around each tooth using a periodontal probe — the most direct way to assess disease presence and severity.
X-RAYS WHEN INDICATED
Dental X-rays can reveal bone levels around tooth roots — important for distinguishing gingivitis (no bone loss) from early or established periodontitis.
TREATMENT DISCUSSION
A clear conversation about whether this looks like early gingivitis or more advanced disease — and what the recommended treatment path involves before you commit to anything.
Treatment Depends on What the Exam Shows
EARLY GINGIVITIS
Inflammation limited to gum tissue · No bone loss
- Professional cleaning to remove plaque and tartar above and just below the gumline
- Personalised home care guidance — technique, tools, and frequency
- Follow-up to confirm tissue has responded well
- Return to regular preventive schedule once stable
MORE ADVANCED DISEASE
Deeper pockets · Bone involvement · Periodontitis
- Scaling and root planing — a deep cleaning below the gumline to remove deposits from tooth roots and periodontal pockets
- Localised antibiotics in some cases, depending on severity
- More frequent periodontal maintenance appointments (every 3–4 months) to keep disease controlled over time
- Specialist referral if needed for advanced cases
Is a Deep Cleaning Painful? What to Expect
Patients ask about this all the time — and the honest answer is: it depends on the level of inflammation and the amount of treatment needed.
Scaling and root planing is more involved than a routine cleaning, but it’s a standard non-surgical treatment for gum disease. Comfort can be managed with local anaesthesia when appropriate. Some tenderness afterward is normal, typically
improving within a few days. Most patients find the procedure far more manageable than they expected — especially when inflammation is caught at an earlier stage.
The better framing: treating gum disease early is usually more manageable than waiting until the condition becomes more advanced and requires more intensive care.
Gum Health and Whole-Body Health
Gum disease is not “just cosmetic.” Research has found associations between periodontal disease and certain systemic conditions — though it’s important to be accurate about what the evidence does and doesn’t show.
Diabetes & Blood Sugar
The strongest and most consistently supported relationship. People with diabetes are at higher risk for periodontal disease, and gum inflammation can make diabetes harder to manage. The relationship works in both directions.
Cardiovascular Disease
Research has found an association between periodontal disease and cardiovascular disease — though the causal relationship is less clearly established. Chronic oral inflammation is worth managing regardless.
BEING ACCURATE ABOUT THE EVIDENCE
The association between gum disease and systemic conditions is real and worth taking seriously. However, it would be too strong to claim that treating gingivitis directly prevents heart disease or other medical outcomes. What’s clear is that chronic oral infection is not something to dismiss — and managing it is part of overall health, not just dental health.
When to See a Dentist vs. a Periodontist
Most early bleeding-gum cases start with a general dentist — and that’s the right first move for most patients. A periodontist is a specialist with advanced training in gum disease and the supporting structures of the teeth.
- START WITH A GENERAL DENTIST
- Gingivitis and most early periodontal concerns
- Routine cleanings and gum disease screening
- Scaling and root planing for mild to moderate disease
- Ongoing periodontal maintenance after treatment
- Determining what level of care is appropriate and whether referral is needed
- SPECIALIST REFERRAL MAY MAKE SENSE FOR
- Significant bone loss on X-ray
- More advanced or complex periodontitis
- Surgical needs — flap surgery, bone grafting
- Recession requiring specialised correction
- Cases that don't respond well to initial non-surgical treatment
Frequently Asked Questions
Why do my gums bleed when I brush or floss?
Are bleeding gums always a sign of gingivitis?
What is the difference between gingivitis and periodontitis?
What is a deep cleaning and is it painful?
Can gum disease affect my heart health or diabetes?
Can gingivitis be reversed at home?
CONCERNED ABOUT BLEEDING GUMS?
Book a gum health evaluation at Toothology in Williamsburg. We’ll measure pocket depths, assess recession, and give you an honest picture of what’s happening.
DIRECT LINE
IN THIS GUIDE
QUICK DECISION GUIDE
A repeated pattern — not a single episode — is the cue to get checked.
TOOTHOLOGY DENTAL
Williamsburg, Brooklyn, NY
Serving Greenpoint, Bushwick, Bed-Stuy & Downtown Brooklyn
718-678-3800
Emergency line available
Open Hours
Mon – Thu: 10:00 AM – 6:00 PM Friday: 10:00 AM – 2:00 PM Sunday: 10:00 AM – 2:00 PM Saturday: Closed
OUR COMMITMENT
- Board-Certified Pediatric Dentists
- Child-Friendly, Anxiety-Reducing Care
- Same-Day Emergency Slots
- Low-Radiation Digital X-Rays
- Most Major Insurance Accepted
